Dementia pugilistica, first found in boxers in the early 20th century, and chronic traumatic encephalopathy, a newer diagnosis, are considered to be the same condition. The effects of chronic traumatic encephalopathy have been extensively researched. It affects certain retired pro or college footballers and other sportspeople who have suffered repeated head trauma and some soldiers who have suffered brain damage as a result of blast trauma.
It’s unclear why only some persons with repeated head trauma acquire chronic traumatic encephalopathy and the risks after varying degrees of head trauma (e.g., how many, how much force). Chronic traumatic encephalopathy affects around 3% of athletes who have experienced many (even seemingly mild) concussions.
In chronic traumatic encephalopathy, hyperphosphorylated tau protein is deposited as neurofibrillary tangles in the microvascular gaps, cerebral sulcal depths, and subpial and periventricular locations.
In this guide, we will discuss in-depth about what CTE is and its causes, stages, symptoms, and treatments available. So let’s get into it without further delay.
CTE
Chronic traumatic encephalopathy (commonly known as CTE) is an uncommon progressive neurodegenerative ailment (i.e., a condition that causes damage to nerve cells (neurons), affecting their function and/or causing them to die). It is assumed to be the result of repeated head trauma over time.
Multiple head traumas or injuries are linked to delayed alterations in the brain, affecting a person’s ability to operate normally. Neurodegenerative alterations tend to develop over time, with clinical symptoms appearing years or even decades after repeated head injuries. These alterations have an impact on how the individual feels, thinks, behaves, and/or moves.
The earliest mention of this syndrome in literature appears to be in the 1920s, when problems in professional boxers’ behavior, cognitive (thinking processing), and motor (movement) capacities were recognized. As a result, the disease was dubbed “punch drunk syndrome” in early literature.
This phrase was eventually renamed dementia pugilistica, which was less derogatory. The term ‘traumatic encephalopathy’ was also employed in several studies, which refers to brain injury in a broad sense. Finally, in the 1960s, doctors coined the phrase “chronic traumatic encephalopathy.”
Physicians began to realize that similar anomalies may afflict a far broader number of people, not only professional boxers, over the next several decades. As additional examples have emerged throughout time, literature has identified the following as possible possibilities in the genesis of the condition:
- Activities like contact sports – American football (NFL), rugby, soccer, hockey, and even professional wrestling.
- Military veterans who have been exposed to warfare, including injuries acquired as a result of blast activity.
- Domestic violence and abuse victims
- Those who indulge in self-inflicted head-banging as a consequence of an underlying illness or as a result of an epileptic episode.
This raises issues about what kind of head/brain injury eventually causes CTE and if the impact’s severity and subsequent damage play a role.
Factors That Contribute to the Development of Chronic Traumatic Encephalopathy Include
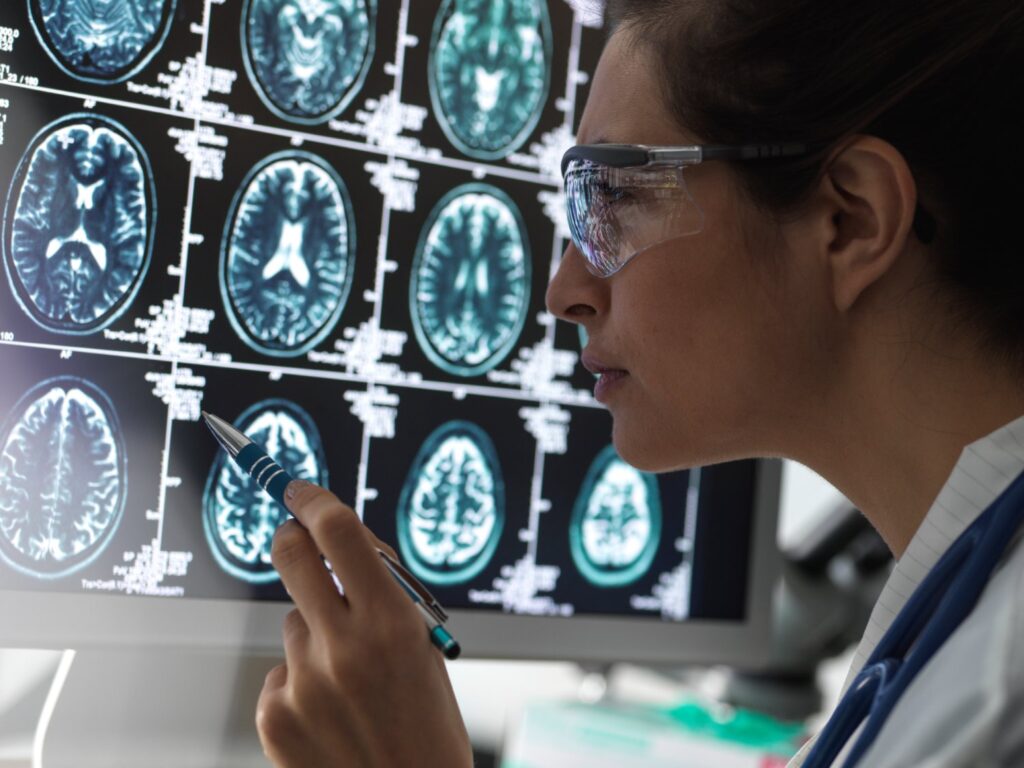
The repetitive impact appears to be a constant factor in the emergence of chronic traumatic encephalopathy. Researchers and medical experts cannot rule out the possibility that such occurrences may increase the chance of neurological impairment later in life, no matter how little, moderate, or severe the impact. Finding straight connections is the key.
1. Traumatic Brain Injury (TBI)
This happens when aberrant brain function is discovered (via diagnostic techniques) after a strong head impact, resulting in temporary or permanent problems. For example, direct collision, item penetration, blast waves, or even something that causes quick brain movement within the skull can all produce harm from an external force.
Acute traumatic brain injury can be fatal. TBI is classified as mild, moderate, or severe depending on how long a person was unconscious at the time of the incident and how long post-traumatic amnesia remained.
Chronic traumatic brain injury, often known as post-concussion syndrome (PCS), can cause cognitive and physical impairments. It might potentially have a role in the progression of chronic traumatic encephalopathy.
2. Concussion
A concussion is a type of mild traumatic brain injury (mTBI) that causes cognitive, behavioral, physical, and emotional changes in the days and weeks following the event. A concussion is described as a temporary change in brain function caused by an external force. However, continual irregularities might last for several months.
A prolonged headache, coordination problems, disorientation, confusion, nausea, vomiting, dizziness, exhaustion, and sleep abnormalities are all symptoms of concussion.
CTE is clinically connected to the long-term consequences of diagnosed mTBI. Chronic symptoms include cognitive, behavioral, emotional, and motor impairments that are comparable to those associated with CTE (which may be found during later study/diagnosis).
3. Repetitive Head Trauma
At this time, recurrent sub-concussive episodes with subclinical consequences (i.e., asymptomatic occurrences) cannot be ruled out as a role in the formation of CTE later in life.
‘Sub-concussive head impact‘ refers to injurious contact, bumps, or blows to the head that may not cause clinical symptoms but can still set off a chain reaction of neurodegenerative changes.
As a result, while not all knocks and blows elicit clinical manifestations at the time of impact, they can nevertheless cause injury, particularly if many stressful events occur.
Symptoms of Chronic Traumatic Encephalopathy/CTE

CTE symptoms may not develop for years after someone has suffered brain damage. However, several of the symptoms are comparable to those of Alzheimer’s disease and Parkinson’s disease, which are both degenerative brain diseases.
Symptoms Associated With Thinking
- Learning challenges
- Loss of memory
- Concentration problems
- Making decisions might be tough due to misunderstandings
- Driving problems
- Lack of direction sense
- Headache or pressure with brain fog
- Disturbance of sleep patterns
- A lack of awareness of experiencing issues
A person’s sleep may also be disturbed if they have experienced a head injury. In addition, sleep deprivation can exacerbate cognitive issues.
Symptoms Associated With Mood
- Agitation
- Suicidal thoughts or depression
- Anxiety
- Fear
- Impulsive behavior
- Lack of empathy
Behavioral Symptoms Include
- Road rage
- Restlessness
- Motivation loss
- Decreased socialization
- Wandering
- Slow movement or changes that resemble Parkinson’s disease
Stages of CTE
Researchers from Boston University outlined four phases of CTE based on the degree of aberrant protein accumulation in patients’ brains in a 2012 study. More severe symptoms distinguish the four phases.
- Stage I- Headaches and trouble with focus and concentration are common symptoms of this period.
- Stage II- Signs of the second stage include those of the first and also short-term loss of memory, sadness, and erratic emotions.
- Stage III- Planning, organization, multitasking, and other cognitive challenges are all symptoms of this stage.
- Stage IV- Memory issues become more acute in stage IV. Dementia frequently follows. Aggression may also become more prominent when cognitive and emotional disorders worsen. In this period, suicidal conduct is also frequent.
Diagnosis of CTE
There are no assessments or diagnostics that can identify CTE at this time. The aberrant accumulation of particular proteins on the surface is the key to detecting the condition.
Unfortunately, there are no existing imaging or laboratory tests that can detect protein clusters. Researchers are working hard to develop diagnostic methods, but CTE can only be identified after death by studying brain matter directly.
Treatment And Management
Good CTE dementia management involves having a primary care physician who can coordinate care. A professional may decide to track a patient’s development over time in order to determine the consistency of their symptoms and reassure them.
Alcohol and smoking are two things to avoid if you want to improve your brain. If you’re having trouble sleeping, try obtaining a sleep test and addressing problems like obstructive sleep apnea. Again, it is critical that family members acquire knowledge and support in order to provide the best possible assistance.
Ways to Prevent CTE
CTE can only be averted totally by avoiding head trauma. Because no one knows the exact criteria for developing the condition, it’s hard to estimate how many head traumas are too many over how long.
You can lower your risk by doing the following steps:
- Eliminate contact sports and other circumstances where a head injury is a possibility.
- If you engage in dangerous activities, always wear appropriate safety equipment and observe all safety regulations and recommendations.
- If you suffer a head injury, make sure you treat it properly according to medical recommendations. After the initial head injury, take care to avoid subsequent ones.
Tips For Caregivers
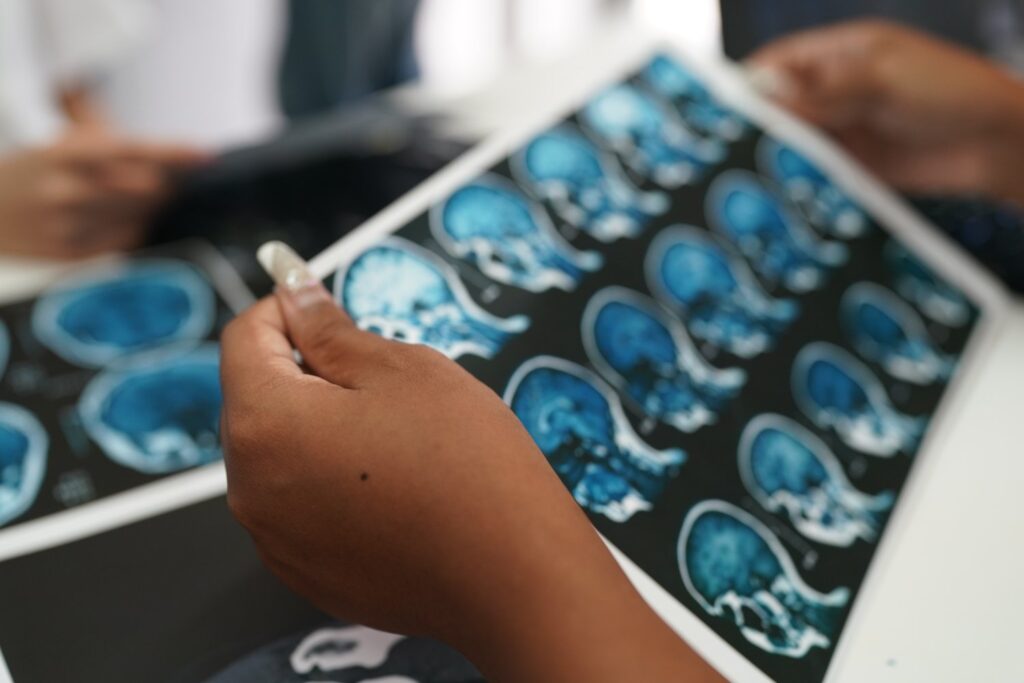
You can assist your loved ones to operate more effectively if they have symptoms that are consistent with CTE. You can also consider programs to support yourself to deal with the disease’s effects, which grow more difficult to manage as time goes on.
1. Learn Everything You Can About the Condition And How it Affects People
Understanding beforehand what to expect as the condition advances will help you manage the worsening symptoms.
2. Assist Your Loved One in Developing Routines
If your loved one has a pattern of regular routines and memory aides, the cognitive and memory impairments that occur with CTE can be controlled more successfully. A soothing routine can also assist you in coping with mood changes and behavioral shifts.
3. Keep the Risks in Mind
Advanced CTE is considered to cause both violent and suicidal behavior. So be on the lookout for these signs and take action to protect your loved one and yourself.
4. Seek Assistance For Yourself
Like all degenerative brain illnesses, CTE has a negative impact on caretakers. So when you feel overwhelmed, don’t be afraid to take a break and seek assistance from other carers and loved ones who are struggling with the sickness, either locally or online.
Takeaway
Repeated head trauma appears to be the cause of chronic traumatic encephalopathy (CTE), a degenerative brain illness. Because CTE cannot be clearly identified in a live patient, it is one of the most poorly known brain illnesses. Only after death, when the patient’s brain matter is studied during an autopsy, can the illness be diagnosed.
It’s impossible to assess the disease’s etiology, symptoms, or prognosis since researchers can’t have a clear look at CTE in living people. CTE appears to be connected to several brain injuries and takes years to manifest. It does not look like the result of a single head injury. However, it is unclear how many brain injuries put a person at risk for CTE over time.
You could be concerned about somebody you know who is exhibiting unusual thoughts, moods, or behavior. Begin by gently asking them to get a memory exam with their doctor.
It’s critical to demonstrate compassion for yourself and others as a friend or family member of someone with CTE dementia and care for your own well-being.
The way you speak or engage with someone who has CTE dementia might help them respond better. A psychologist or occupational therapist with experience in brain injuries can aid with role-playing.
References
- https://www.dementia.org.au/about-dementia/types-of-dementia/chronic-traumatic-encephalopathy-dementia
- https://www.msdmanuals.com/en-in/professional/neurologic-disorders/delirium-and-dementia/chronic-traumatic-encephalopathy-cte
- https://www.mymed.com/diseases-conditions/chronic-traumatic-encephalopathy-cte
- https://unitedbrainassociation.org/brain-resources/chronic-traumatic-encephalopathy/



